A hemorrhoid is a common illness that numerous Minnesotans suffer from. Approximately three out of four people will develop hemorrhoids at some time in their lives. While many people associate hemorrhoid treatments with painful surgery, only a small percentage of hemorrhoid patients actually require hemorrhoidectomy. A fast and simple non-surgical office procedure has taken the fear out of hemorrhoid treatments. The majority of hemorrhoid patients are good candidates for non-surgical Infrared coagulation (IRC) treatments.
What is Infrared Coagulation (IRC)?
IRC is a FDA approved office procedure that uses infrared light to treat symptomatic internal hemorrhoids, and it takes just a couple of minutes for each treatment. IRC is a safe, fast, and effective solution for hemorrhoids. Therefore, IRC has quickly become the most widely used office procedure for hemorrhoid clinics and is preferred over other methods because it is fast, effective, well-tolerated by patients, and rarely has complications.
A small light probe contacts the area above the hemorrhoid complex under direct view, exposing the tissue to a burst of infrared light for about 1.5 second. This coagulates the veins above the hemorrhoid, causing it to shrink.
With IRC, hemorrhoid doctor can effectively coagulate the insensitive area right above the hemorrhoids and destroy these small veins. In this way, the sensitive and painful area is avoided, and IRC becomes a very tolerable treatment.
IRC offers major advantages to patients over previous hemorrhoid treatment methods:
• Fast, simple, and safe solution
• No anesthesia required
• No special preparation needed
• No recovery time after treatment
• Clinically proven results
• Covered by all major insurance companies
Who are the Best Candidates for Infrared Coagulation (IRC)?
Infrared coagulation can be used to treat the early stages of hemorrhoids, and it is most effective in grade 1-2 hemorrhoids.
How is Infrared Coagulation Procedure Performed?
Before IRC procedure is performed, Dr. Shu gently inserts the anoscope (a very short, 3-4 inch rigid metal tube), then uses a handheld device that creates an intense beam of infrared light to touch the mucosa above the hemorrhoids, exposing the hemorrhoid tissue to a quick pulse of infrared light. The heat from the infrared light burns 4-5 spots in the targeted area, coagulating the vein above the hemorrhoids.
The resulting scar tissue cuts off the blood supply to the hemorrhoid venous complex. This causes the hemorrhoid complex to shrink and die. It may take a few weeks for all the hemorrhoids to shrink completely. Moreover, the scar tissue acts to hold nearby hemorrhoid veins in place so they don’t bulge into the anal canal easily and become hemorrhoids as you age.
Each IRC treatment only takes a couple of minutes. You may need as many as four separate treatment sessions every two weeks to cover all the areas where hemorrhoids appear, but this depends on each individual case and how extensive your hemorrhoids are.
What is the Recovery Time of Infrared Coagulation Procedure?
After the IRC procedure, you may feel mild discomfort in the anus and the urge to have a bowel movement sometimes. You are able to resume normal everyday activities immediately afterward. Typically, there are no post-treatment effects. However, there may be slight spot bleeding a few days later, but heavy rectal bleeding is extremely rare. Avoid heavy straining, lifting, and aspirin. If you notice significant rectal bleeding, you should call your doctor’s office.
You may use Tylenol as needed and take a warm sitz bath daily to relieve discomfort. A stool softener, fiber, and water will help ease your bowel movement while you heal.
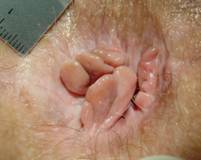 Anal skin tags often occur if an individual heals the thrombosed external hemorrhoids at home without surgery, the thrombosed hemorrhoids may leave behind skin tags. Anal sentinel tags may also form because of non-hemorrhoid causes, such as anal fissure, surgery, or infection, etc.
Anal skin tags often occur if an individual heals the thrombosed external hemorrhoids at home without surgery, the thrombosed hemorrhoids may leave behind skin tags. Anal sentinel tags may also form because of non-hemorrhoid causes, such as anal fissure, surgery, or infection, etc. 


