Sebaceous cyst (Epidermoid cyst)
Sebaceous cysts are small bumps that develop just beneath the skin on your face, neck, trunk and sometimes your genital area. They are slow-growing and often painless.
Sebaceous cysts are almost always noncancerous, but in rare cases, they can give rise to skin cancers. Because this occurs so seldom, sebaceous cysts usually aren’t biopsied unless they have unusual characteristics that suggest a more serious problem or big enough to be removed.
Sebaceous cysts:
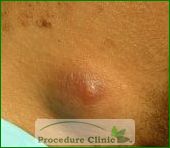
- Are round cysts or small bumps that are that are attach to the skin.
- Are usually white or yellow, though people with darker skin may have pigmented cysts
- Range in size from less than 1/4 inch to nearly 2 inches in diameter
- May have a central opening that’s plugged by a tiny blackhead.
- Occur on nearly any part of your body, including your fingernails, but are found most often on your face, trunk and neck.
- Infection can occasionally occur, include thick, yellow material draining from the cyst that may have a foul odor and redness, swelling and tenderness around the cyst.
Causes
Sebaceous cysts form out of your sebaceous gland under skin. The sebaceous gland produces the oil called sebum that coats and lubricates your hair and skin. Cysts can develop if the gland or its duct, the passage where oil is able to leave, becomes damaged or blocked. This usually occurs due to a small trauma to skin.The small trauma may be a scratch or a skin condition, such as acne. Sebaceous cysts grow slowly, so the trauma may have occurred months before you notice the cyst.
Other causes of a sebaceous cyst may include:
a misshapen or deformed duct
damage to the cells during a surgery
genetic conditions, such as Gardner’s syndrome or basal cell nevus syndrome
Complications
In rare cases, sebaceous cysts can give rise to basal and squamous cell skin cancers. Because this occurs so seldom, Sebaceous cysts usually aren’t biopsied unless they’re solid, immobile, infected or have other unusual characteristics that suggest a more serious problem.
Besides cancer, other complications include:
- Inflammation. Sebaceous cysts can become tender and swollen, even if they’re not infected. Inflamed cysts are difficult to remove, and your doctor is likely to postpone treating them until the inflammation subsides.
- Rupture. A ruptured cyst often leads to a boil-like abscess that requires prompt treatment.
- Infection. An sebaceous cyst can become infected spontaneously or after a rupture.
Treatments and drugs
Small cysts that don’t cause cosmetic or functional problems are usually left alone. When a cyst is inflamed, gets bigger, ruptured or infected, these treatment options exist:
Incision and drainage: your doctor makes a small cut in the cyst and expresses the contents. Although incision and drainage is relatively quick and easy, cysts often recur after this treatment.
Total excision: The surgical excision removes the entire cyst and so prevents recurrence. Excision is most effective when the cyst isn’t inflamed. Your doctor may recommend first treating the inflammation with antibiotics, steroids, or incision and drainage and then waiting to perform excision for four to six weeks after inflammation resolves. Total excision requires sutures. Your doctor will remove sutures in your face within a week or so of total cyst excision, and will remove sutures elsewhere in your body within a week.
Minimal excision: Some doctors prefer this technique because it removes the whole cyst wall but causes minimal if any scarring. During the procedure, your doctor makes a tiny incision in the cyst, expresses the contents, and then removes the cyst wall through the incision. The small wound is usually left to heal naturally.
Ganglion cysts are noncancerous fluid-filled lumps (cysts) that most commonly develop along the tendons or joints of your wrists or hands. They may also appear in your feet. A ganglion cyst may develop suddenly or gradually over time. The exact cause is unknown.
In many cases, ganglion cysts will cause you no pain and require no treatment. Often, they go away on their own. When you do need treatment for a ganglion cyst — due to pain or interference with joint movement or for cosmetic concerns — it usually consists of removing the fluid from the ganglion cyst or surgically removing the cyst.
Ganglion cysts generally are:
- Raised lumps near your wrist or finger joints
- Round, firm and smooth
- Fluid-filled, as evidenced by shining a light through the cyst (transillumination)
- Variable in size depending on your activity level, becoming larger when you use the affected joint and growing smaller when you’re at rest
- Painless, although in some cases the cysts may put pressure on the nerves near the joint, which can cause pain, weakness or numbness.
In some cases, the telltale lump that usually indicates a ganglion cyst isn’t visible. Often the only indication of these smaller, “hidden” ganglion cysts (occult ganglions) is pain. These occult cysts can be seen only with ultrasound or MRI.
Causes
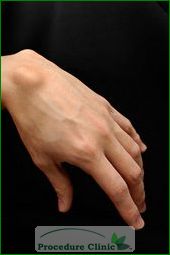
It’s not clear what causes a ganglion cyst to develop. It grows out of a joint, similar to a balloon on a stalk, and seems to occur when the tissue that surrounds a joint or a tendon bulges out of place. Inside the cyst is a thick fluid similar to that found in joints or around tendons.
Treatments and drugs
Small ganglion cysts are often harmless and painless, requiring no treatment. In fact, in many cases, doctors recommend a watch-and-wait approach before exploring treatment options. However, if the ganglion cyst is causing pain or it’s interfering with joint movement, your doctor may recommend one of several treatment options.
Immobilization: Because activity can make the ganglion cyst grow larger, your doctor may recommend wearing a wrist brace or splint to immobilize the area. This helps your hand and wrist to rest, which may help shrink the cyst. As the cyst shrinks, it may release the pressure on your nerves, relieving pain.
Aspiration: your doctor drains the fluid from the cyst. To do so, your doctor applies a local anesthetic to the area above the cyst. Then, he or she punctures the cyst with a needle and removes the fluid from the base of the cyst with a syringe. Your doctor may recommend a steroid injection into the empty cyst after aspiration. This procedure can be done right in your doctor’s office.
After aspiration, as many as 60 percent of ganglion cysts may recur. If the cyst recurs, aspiration can be repeated. However, in some cases your doctor may recommend surgery to remove the cyst.
Surgery: If you have significant pain or difficulty with joint movement, or if other treatments aren’t working, your doctor may recommend surgery to remove the ganglion cyst. In most cases, doctors perform the surgery on an outpatient basis, which means you’ll go home the same day as the operation.
During surgery
- Typically, a local or regional anesthetic is used to numb the affected area.
- The surgeon then makes an incision in the skin overlying the ganglion cyst. The size of the incision depends on the size of the cyst.
- The surgeon removes the cyst and the stalk that attaches it to the joint or tendon, along with a small portion of the surrounding tissue in most cases.
- Then the surgeon will stitch and bandage the affected area.
After surgery
- Keep the affected limb elevated for up to 48 hours to help reduce swelling. You may experience discomfort, swelling and tenderness for two to six weeks.
- Your doctor may recommend analgesics, such as acetaminophen (Tylenol, others), or nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil, Motrin, others) or naproxen (Aleve, Naprosyn, others), for pain relief.
- Change your bandages (dressings) as directed.
- Depending on the location of the cyst, your doctor may recommend temporarily wearing a splint or brace to help minimize postoperative pain. In most cases, however, moving the affected area soon after surgery is recommended.
- As the incision heals, it’s important to watch for signs of infection, including redness, swelling or discharge.
- Usually, physical therapy is not necessary after ganglion cyst removal. But if you have new problems with joint stiffness, therapy may help you regain strength in your hand, wrist or foot.
Unfortunately, there’s no guarantee that a ganglion cyst won’t recur, even after surgery. And as with all surgeries, there are risks to be considered. Though rare, injury to nerves, blood vessels or tendons may occur. These could result in weakness, numbness or restricted motion. Your doctor can help you decide the best treatment for you.
.JPG)



