Hemorrhoids Online Registration
Every year, hundreds of thousands of individuals are diagnosed with colon or rectum cancer. Although anorectal symptoms and complaints are common and typically not a serious concern, all patients should be examined for signs of possible cancer. Common symptoms of anorectal disease include rectal pain, bleeding, anal itching, and rectal mass or lump.
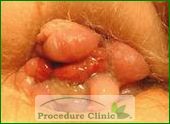
Patients should be checked for anorectal disease as early as possible if symptoms arise. If caught in its early stages, the cancer will require less extensive treatment and stress to the patient. Patient assessments must include an anorectal exam, flexible sigmoidoscopy or colonoscopy. For colorectal cancer, patients 50 years of age or older in the general population and 40 years of age or older with risk factors or a family history of the disease should begin regular screenings.
Anal/Rectal Anatomy
The anus is the outlet to the gastrointestinal tract, and the rectum is the lower 10 to 15 cm of the large intestine. The dentate line divides the outer skin from the mucosa. Four to eight anal glands drain into the crypts of Morgagni at the dentate line; most rectal abscesses and fistulae originate in these glands. The area of the rectum above the dentate line does not contain pain nerves, which allows for surgical procedures to be performed without anesthesia. However, the area below the dentate line is highly sensitive. Bowel movements are controlled by the muscles of both the involuntary internal sphincter and the voluntary external sphincter.
Anorectal Examination
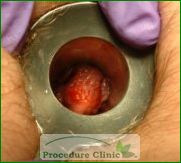
Anorectal assessments include inspection, palpation and anoscopic examination. The patient typically lies sideway on his or her left side, which is allows comfort for the patient as well as good visualization and access for the examiner. The doctor often finds the external hemorrhoids, anal polyp, and anal fissure or fitstula by simple inpection. The digital exam is to palpate any suspicious mass lesion in the anorectal canal. Anoscopy is to confirm the diagnosis of hemorrhoids, anal fissure and other anorectal diseases.
Common Anorectal Symptoms
Anal Itching
Anal itching is a common symptom, but initial relief of the itching does not necessarily mean the problem goes away. Continuous scratching or excessive cleaning of the anal area may further harm the sensitive tissues and worsen symptoms. In addition, the area can be highly sensitive to perfumes, soaps, fabrics, dietary intake and superficial trauma. When chronic itching occurs, the perianal area becomes white with fine fissures.
Treatments for anal itching include taking antihistamine as a sedative prior to sleeping to prevent the patient from unconsciously scratching, or using a topical corticosteroid to alleviate the itching. Underlying disorders such as hemorrhoids must be considered and treated when diagnosing and treating anal itching.
Anal pain
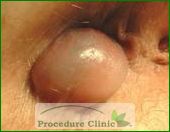
Anal pain is a common sign of anorectal disease. Pain caused by an acute anal fissure may occur during intense, forced bowel movements that are often accompanied by rectal bleeding. Pain that begins gradually and becomes excruciating may indicate infection, and occurrence of fever and inability to urinate indicates need for emergency treatment. Immediate onsets of intense pain accompanied by a palpable mass are usually a result of an external thrombosed hemorrhoid, which may last a few days to a couple of weeks. Internal hemorrhoids, however, are not painful due to being located above the dentate line of the rectum. Similarly, rectal cancer typically does not cause pain unless the condition is advanced. The patients with chronic anal fissures usually have intermittent sharp rectal pain and bleeding with each bowel movement for a long time.
Proctalgia fugax is a more serious anal pain condition that involves short spasms of intense pain at night. This condition may occur once each year or up to three or four times each week. The pain is typically accompanied by sweating and an urge to pass stool. There is currently no treatment for proctalgia fugax, but placing oneself in hot water or applying ice may provide symptomatic relief.
Lump/palpable mass
A palpable mass in the anal area may or may not indicate cancer or hemorrhoids. Lumps can be caused by a variety of conditions including anal warts, hemorrhoids, polyps, fissures, or cancer.
Rectal bleeding
Rectal bleeding can be caused by various conditions, but even the slightest amount of bleeding should be taken seriously. Common causes of bleeding are hemorrhoids, fissures and polyps. Patients of older age or with significant family history of bowel disease or cancer should consider further examination. In addition, patients who were previously treated for rectal bleeding but continued to experience bleeding must be further examined.
Common Anorectal Diseases
Anal warts
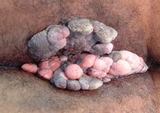
Anal warts are caused by the human papillomavirus (HPV), which has been linked to increased risk of cervical and anal cancers. Infection occurs when secretions collect in the anal area, causing multiple warts of various sizes. Although individuals who engage in anal intercourse have a higher frequency of perianal warts, the majority of patients with perianal warts have not engaged in anal intercourse.
Anal warts can be treated with agents such as topical Fluorouracil (Efudex) and Imiquimod (Aldara), but they have a low cure rate. Trichloroacetic acid (TCA) and cryotherapy with liquid nitrogen are more successful but may require several treatments, especially with large lesions. Radiofrequency and laser therapy produce 90 percent cure rates and is the preferred treatment method by Dr.Shu.
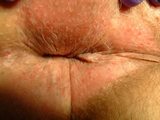
Fissures
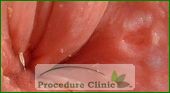
A fissure is a small cut or split in the anoderm often caused by a painful, hard bowel movement. Pain from the bowel movements usually lasts for about an hour before either subsiding or continuing at a lesser degree. Fissures are typically located anterior or posterior to the anus. When fissures are found laterally, other uncommon causes should be considered.
Treatment for an acute fissure is quite simple when it is identified within a month of onset. 85% to 90% patients respond well to anal care measures. Once a fissure has become chronic,, it is more difficult to treat. Topical solutions such as nifedipine gel or nitroglycerin ointment have about 50 percent success rates. Most patients couldn’t tolerate the headache side effect from nitroglycerin ointment. Chronic fissures are usually treated with lateral sphincterectomy, a surgical office procedure that cures 90-95% of cases. A chemical sphincterectomy using a botox injection into the anal sphincter is an alternative option.
Anal fistula
Anal fistulas are usually caused by an abscess in the anal area due to infection. Patients often experience recurrent infection with intermittent drainage of pus from the anal’s opening. Abscess formation can be easily treated using incision and drainage (I&D), antibiotics, and frequent Sitz baths.
Patients with chronic complicated fistulas are treated with a fistulotomy or fistulectomy, including cutting setons, advancement flaps or muscle repair and fibrin glue injection.
Anal abscesses
Abscesses also begin as an infection in the anal glands. The patients usually have severe rectal pain with local redness and swelling. Superficial perianal abscesses are easily drained in the office under local anesthesia, it resolve after treated with antibiotics and anal care measures.
The infection may track through the sphincter muscles to enter the surrounding space or above levator muscle. The patients usually have toxic signs and fever. and these abscesses are difficult to diagnose and require a high index of suspicion.
Hemorrhoids
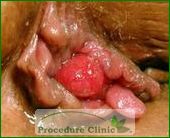
There are three types of hemorrhoids – internal, external, and mixed. Internal hemorrhoids form above the dentate line, while external hemorrhoids form below the dentate line. Mixed hemorrhoids can either refer to lesions formed at the dentate line, or to the presence of both internal and external hemorrhoids.
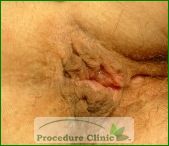
External hemorrhoids are those occur outside the anal verge. External hemorrhoids usually affect the cleansing after the bowel movement and cause the skin irritation and itching. The thrombosed external hemorrhoids are sometimes very painful if the varicose veins rupture and the blood clots develop, it is often accompanied by swelling and irritation. These hemorrhoids are typically treated with either incision and removal of the clot or with external hemorrhoidectomy. Simply draining the clot can lead to recurrence, so it is generally recommended to completely excise the thrombosed hemorrhoids.
Internal hemorrhoids are graded from I to IV based on the degree of prolapse. Grade I lesions bulge with defecation; grade II lesions also bulge with defecation but then recede spontaneously. Grade III hemorrhoids require digital replacement after prolapsing, while grade IV hemorrhoids cannot be replaced once prolapsed. There are many treatment options for the internal hemorrhoids.
Grade 1: Very early hemorrhoids can often be effectively dealt with by dietary and lifestyle changes. The lifestyle changes should also be part of treatment plan for the more advanced hemorrhoids.
- Eat plenty of fruit, leaf vegetables, and whole-grain breads and cereals
- Use bulk-forming stool softener and fiber supplements such as Metamucil
- Exercise regularly
- Lose weight
- Drinking six to eight glasses a day of water
- Avoid sitting and straining too long while using the restroom
- Avoid reading in the bathroom
- Avoid using soap or toilet paper that is perfumed which may irritate the anal area
- Avoid excessive cleaning, rubbing, or wiping of the anal area
Grade 1-2: Infra-Red Coagulation (IRC) has become the world’s leading office treatment for hemorrhoids. This non-surgical treatment is fast, well tolerated, and remarkably complication-free. A small probe is placed in the base of the hemorrhoid and a few short bursts of infrared light are applied. The infrared light quickly coagulates the vessels that provide the hemorrhoid with blood, causing the hemorrhoids to shrink and recede. Shrinkage of the hemorrhoidal tissues may take a few weeks.
Grade 3: Rubber band ligation is widely used for the treatment of more advanced (more prolapsed) internal hemorrhoids where the prolapsed hemorrhoidal tissue is pulled into a double-sleeved cylinder to allow the placement of two rubber bands around the tissue. Over time, the ligated tissue dies-off. Rubber band ligation usually is performed in the clinic. Often, however, there is the need for more than one procedure to resolve the condition. Rubber band ligation downgrades the hemorrhoids to grade 1 or 2, some patients may need to do Infra-Red Coagulation (IRC) treatments after Rubber band ligation.
Grade 4: A hemorrhoidectomy surgically removes the tissue that causes bleeding or protrusion. It is done in a doctor’s office under anesthesia and may require a period of inactivity.
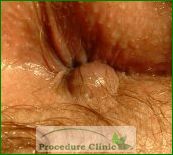
Anal Tags
Anal tags usually arise from previous external hemorrhoids and may periodically cause itching, anxiety or hygienic problems. The tags can be surgically removed using local anesthesia.
Anal Polyps
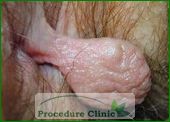
Anal polyps are the growth in the anal canal that must be removed for the biopsy. Further examination with colonoscopy is required for polyps confirmed to be adenomatous in order to check for proximal lesions in the rectum and colon. Hypertrophied Papillae is anal papilla at the dentate line, often confused with a polyp. Treatment is generally not indicated for confirmed hypertrophied papillae.
Cancer of the Anus and Rectum
Anal cancer is account for 2% of cancer in the gastrointestinal tract. Anal or rectal cancer generally do not produce any pain; an external or internal mass may be palpable. Some lesions are so soft that they are missed on palpation. Anal cancers are staged and treated differently from rectal cancers. Anal cancer can take several forms including ulcers, polyps or verrucous growths; treatment is typically a combination of surgery, chemotherapy and pelvic radiation.